Last Updated on January 23, 2026 by Sunit. S. Ekka

A waddling gait is often a sign of weak hip stabilizers. The good news? With targeted physiotherapy exercises, this pattern can often be corrected, improving stability and reducing your risk of pain and injury.
A waddling gait, also known as a myopathic gait, is a way of walking characterized by a side-to-side swaying motion of the hips and trunk. If you can imagine how a duck walks, you will have a good idea of how a person with a waddling gait walks.
But what causes a waddling gait, and how can your physiotherapist help? Let’s find out in this article.
What is a Waddling Gait? (Myopathic Gait)
Waddling gait can be defined as a distinctive walking pattern characterised by lateral tilting of the pelvis and exaggerated side-to-side movements. This pattern differs significantly from normal gait, which is typically smooth and rhythmic.
If we compare it with the normal gait cycle, there is an exaggerated lateral movement in a waddling gait, causing the person to sway from side to side. This abnormal movement pattern arises from difficulties stabilising the pelvis and hip during walking, leading to an observable ‘waddle’.
Clarifying the Terminology: Waddling vs. Trendelenburg
It’s important to know that a waddling gait is different from a similar pattern known as a Trendelenburg gait. According to a review in StatPearls 2, a Trendelenburg gait is a unilateral issue in which the pelvis drops on the opposite side when standing on the weak leg.
A waddling gait, however, is actually a bilateral Trendelenburg gait. This is commonly seen in bilateral conditions like muscular dystrophies or advanced bilateral osteoarthritis.
The Biomechanics: Why a Waddling Gait Occurs
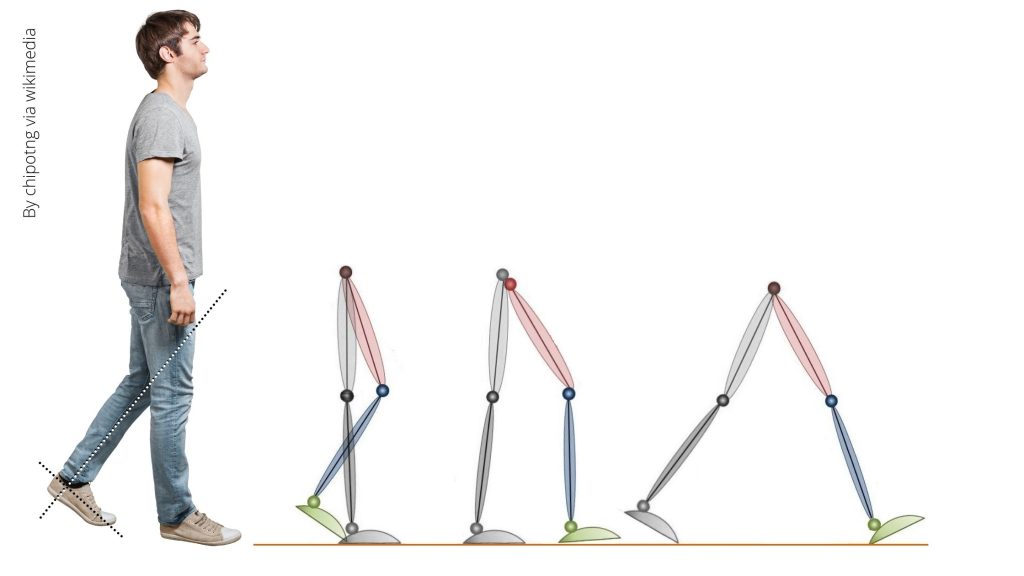
The swing phase is the gait cycle phase immediately after the ‘toe-off’. This phase begins when the foot leaves the ground and ends when it touches down again.
As you can see in the figure below, our reference leg is deep-coloured, and critical changes occur at the hip, knee, and ankle joints during this time.

- The hip flexes to lift the leg,
- The knee then bends to allow the foot to clear the ground and
- At the ankle joint, it dorsiflexes to prepare for the foot’s return to the earth.
These coordinated actions help propel the leg forward, preparing for the next step in the cycle. Any factor that disturbs the rhythm of the swing phase results in an altered gait known as a waddling gait.
Any factor that disturbs the rhythm of the swing phase results in an altered gait. Research shows that hip abductor weakness is a primary disruptor. These muscles are crucial not just for stance but for propelling the trunk medially during late stance to prepare for the swing phase.
When they are weak or fatigued, this “push-off” is less effective, leading to a slower, less stable transition into swing and contributing to the observed pelvic drop and trunk sway5.
Waddling Gait Causes and Associated Conditions
Several factors can lead to an altered swing phase of the gait cycle, resulting in a waddling gait. The reason for one may be completely different from the other. Let us first learn the conditions where the waddling gait is commonly seen.
- Hemiplegia.
- Severe osteoarthritis knee.
- Sciatica.
- Congenital hip dysplasia.
- Muscular dystrophy.
Observe that the waddling gait is seen in paralytic cases such as hemiplegia and pain conditions such as osteoarthritis knee. Both are quite different.
Various medical conditions have been associated with waddling gait, including myopathies (particularly Duchenne muscular dystrophy), bilateral congenital dislocation of the hips, hypothyroidism, and vitamin D deficiency1.
So, what factors lead to a waddling gait?
Factors that cause waddling gait
The two main factors are joint pain and muscle weakness around the thigh and lower leg. These may affect gait in isolation or coexist.
Muscle weakness could be due to hemiplegia, paraparesis, chronic OA knee, etc. The pain conditions could be sciatica or severe bilateral OA knees.
1. Hip Abductor Weakness (The Trendelenburg Mechanism)
In a waddling gait, the primary driver is often severe weakness of the hip stabilisers, particularly the gluteus medius and minimus muscles. This is clinically known as Trendelenburg’s sign.
The hip abductor mechanism acts like a lever; when these muscles are weak, they cannot hold the pelvis level when standing on one leg, causing the pelvis to drop on the opposite side.
Different research provides robust evidence for this mechanism:
- Recovery Depends on Abductor Strength: A 2025 study on patients after hip replacement found that hip abductor strength had a direct impact on functional recovery.
As their strength improved over the course of six months, their walking distance more than doubled, and their balance scores significantly improved4. - Even Temporary Weakness Disrupts Gait: An experimental study from 2015 showed that simply fatiguing the hip abductor muscles in healthy older adults was enough to disrupt their walking.
Immediately after fatigue, participants showed increased step variability, less symmetry between steps, and a slower, more unstable trunk movement5. - Biomechanical Proof: Another study experimentally induced a 33% reduction in hip abductor strength in healthy individuals through stretching.
This immediate weakness directly caused measurable changes in their gait, including increased pelvic drop (obliquity) and greater hip adduction during walking—the classic signs of a Trendelenburg mechanism6.
When this weakness is bilateral, the pelvis sags alternately from side to side with each step, resulting in the characteristic “waddling” pattern.
The body may also compensate by bending the trunk over the weakened hip with each step to maintain balance, a movement known as a “compensated Trendelenburg gait” or “lurch.”
2. Pain and Compensation
I have seen a waddling gait in patients with severe bilateral osteoarthritis knees and sciatica.
It is also seen in total knee replacement cases requiring proper gait training post-operatively and in post-operative hip replacement patients. Here, pain makes the person unable to move, bending in the knee and/or hip joint, leading to an altered swing phase gait cycle.
If the pain is old, the muscle weakness further aggravates the condition.
3. Physiological Adaptation (e.g., Pregnancy)
It’s important to recognize that a waddling-like gait isn’t always pathological. A classic example is the gait change in pregnancy. As pregnancy progresses, the added weight of the growing baby shifts the centre of gravity forward.
Ironically, in this case, according to a study3, waddling gait is found to be actually a protective mechanism and a sign of balance control.
The research showed that:
- Pregnant individuals who adopted a wider step width (a key feature of the waddle) demonstrated a significant improvement in recapturing their balance during walking.
- The study also found that taking these wider steps did not increase the energy cost of walking, meaning it’s an efficient and smart adaptation by the body.
- The researchers concluded that this “waddling gait” increases safety and should be seen as a natural and beneficial response to the physical changes of pregnancy.
Waddling Gait Treatment: The Physiotherapy Approach
So, the weak hip abductor muscle, mainly the gluteus muscle, is the main cause behind the waddling gait45. The principal physiotherapy approach would be the strengthening of this muscle.
There can be many causes for gluteus medius weakness. You can refer to the rehabilitation program for individual conditions such as hemiplegia, myopathy, Total Hip replacement (Osteoarthritis hip exercises), Total knee replacement (Osteoarthritis knee exercises), etc.
Here we will discuss the most common research-backed gluteus medius strengthening exercises that apply to each condition and are effective in strengthening of hip abductors and hence managing the waddling gait7.
1. Double-Leg Bridge

- Lie on your back with knees bent and feet flat. Lift your hips to form a straight line from knees to shoulders.
- Focus: Squeeze your glutes at the top.
- Hold for 5 seconds and then lower it slowly
- Repeat this for a minimum of 20 repetitions.
2. Clamshell (Basic)

- Lie on your side with knees bent and heels together. Keep your hips stacked and feet in contact.
- In this position, lift the top knee. While lifting, make sure not to rock your hip backwards.
- Hold for 5 seconds and lower it slowly.
- Repeat this for 10-20 times in a session.
3. Standing Glute Squeeze (Double-Leg Stance)
We suggest you perform this exercise in standing. If you have a problem in the standing position, then you can also perform this in the prone (lying on your tummy) position. Let’s learn it in a standing position.
- So, stand straight and tall.
- In this position, simply squeeze your glutes together as hard as you can without pain.
- Hold for 5-10 seconds.
- Repeat this for 10 to 15 repetitions.
4. Single-Leg Bridge
The process of performing this exercise is similar to the normal bridging exercise that we just discussed. The only difference is it is performed with a single leg. Here is the step-by-step method to perform this:
- Lie down flat on your back with both hip and knee bent and foot flat on the bed.
- Now, extend one of the legs straight up. This should be your starting position for the exercise.
- In this position, raise your hips to a maximum point.
- Hold this position for 5 seconds and then come to the normal position.
- Repeat this 10 times in a session.
- Perform this same process with the other leg raised.
5. Side-Lying Hip Abduction (Neutral Rotation)

As the name suggests, this exercise is performed in the side-lying position.
- So, lie on your side with legs straight.
- In this position, slowly lift the top leg toward the ceiling, keeping it straight and your toes pointing forward. Do not lift it to more than 30 30-degree angle.
- Hold this position for 5 seconds.
- Now, slowly lower it back to the starting position and then repeat the same process.
- Repeat it for a minimum of 10 repetitions.
6. Standing Hip Abduction (Non-Weight-Bearing)

The starting position for this exercise will be standing with support. You can take support from a table, a wall or anything that is stable.
- Stand straight and hold a wall/chair for support.
- Keeping your leg straight, lift one of your legs to the side without leaning your torso.
- Hold this position for seconds and bring it back to the normal position.
- Repeat this for a minimum of 15 to 20 repetitions.
- Perform the same process with the other leg.
Key Takeaways and When to See a Physiotherapist
Understanding the underlying cause is the first step to effective treatment. As the evidence shows, hip abductor weakness is a central mechanism, whether from neurological events, post-surgical weakness, or pain-induced inhibition.
The research is clear: successful outcomes are achieved by directly addressing this weakness through targeted, progressive strengthening4 and gait retraining to improve stability and symmetry5. Once the underlying cause is addressed, your physical therapist can help you retrain these normal walking patterns.
Keep Reading: New 3D Tech prosthetic liners help more amputees walk again




Pingback: Circumduction gait: Causes, muscle weakness, treatment - Physiosunit
Thanks for the comment sir. My observation says that waddling gait mildly improves in mild OA knee with NSAID on
How common is waddling gait due to OA knee with mild pain managed with NSAID off and on?
Pingback: Gait Cycle Muscles Activity| Anatomy explained - Physiosunit
Pingback: Circumduction gait: Causes, muscle weakness, treatment : Physiosunit
Thank you so much. Have any more questions? please drop a comment
Nice post, Thank you for sharing valuable information. I enjoyed reading this post. The whole blog is very nice found some good stuff and good information here Thanks for sharing…Also visit my page.
Premium Folding Wheelchair